A Pediatric Case Study: Comprehensive Management of Pleural Effusion in a 6-Year-Old Girl
Introduction:
Pleural effusion, an abnormal accumulation of fluid in the pleural space surrounding the lungs, poses significant challenges in pediatric cases. This article delves into the detailed progression and management of a 6-year-old girl who presented to the emergency department with a persistent cough, ultimately diagnosed with pleural effusion. The journey from initial presentation to discharge is illuminated through a series of X-ray images, showcasing the complexity and success of her medical care.
Case Presentation:
Day 1 – Initial Presentation:
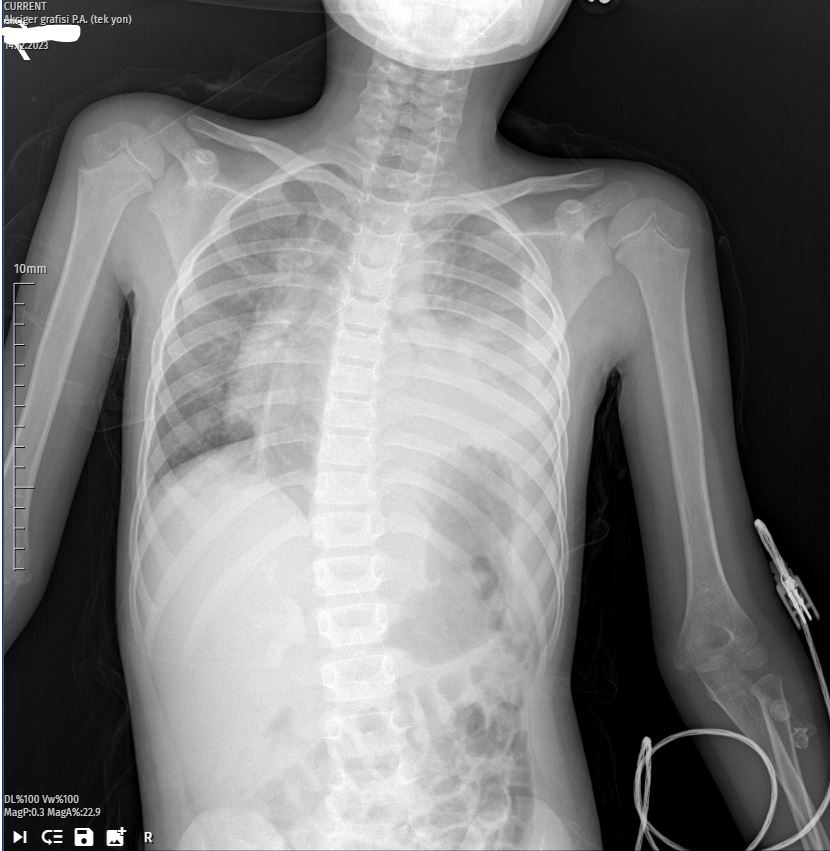
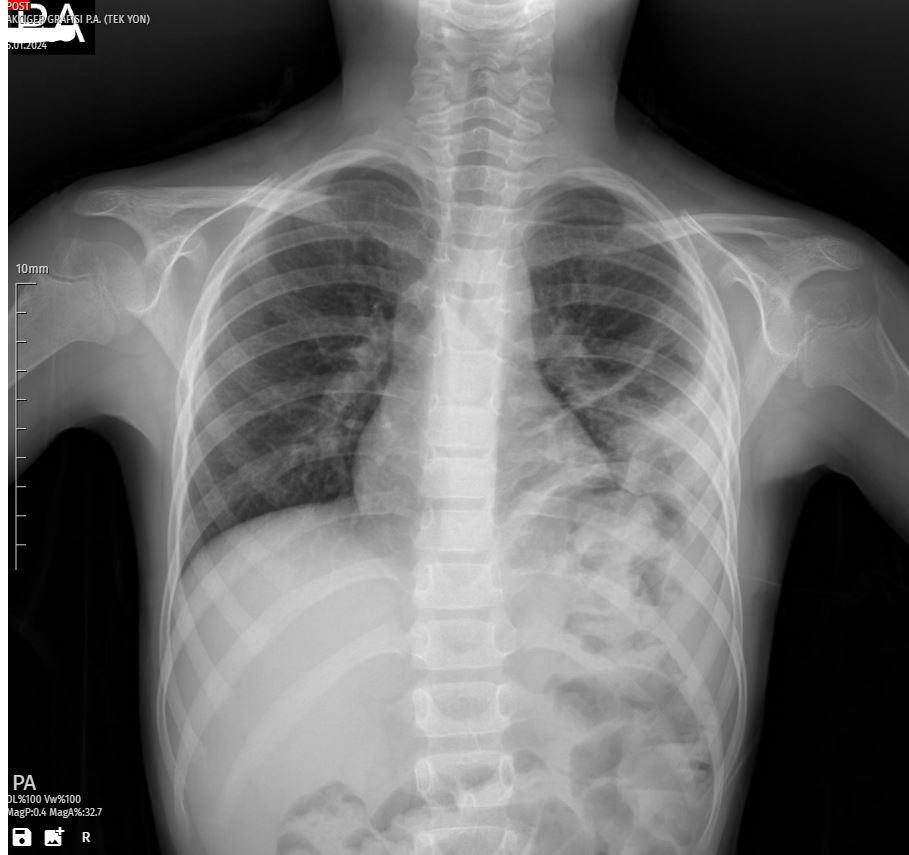
Upon the girl’s arrival at the emergency department, the first X-ray revealed a striking white shadow on her left lung, indicating a substantial pleural effusion. The patient’s persistent cough and the severity of the X-ray findings prompted her immediate admission to the hospital for further evaluation and management.
Day 3 – Worsening Pleural Effusion:
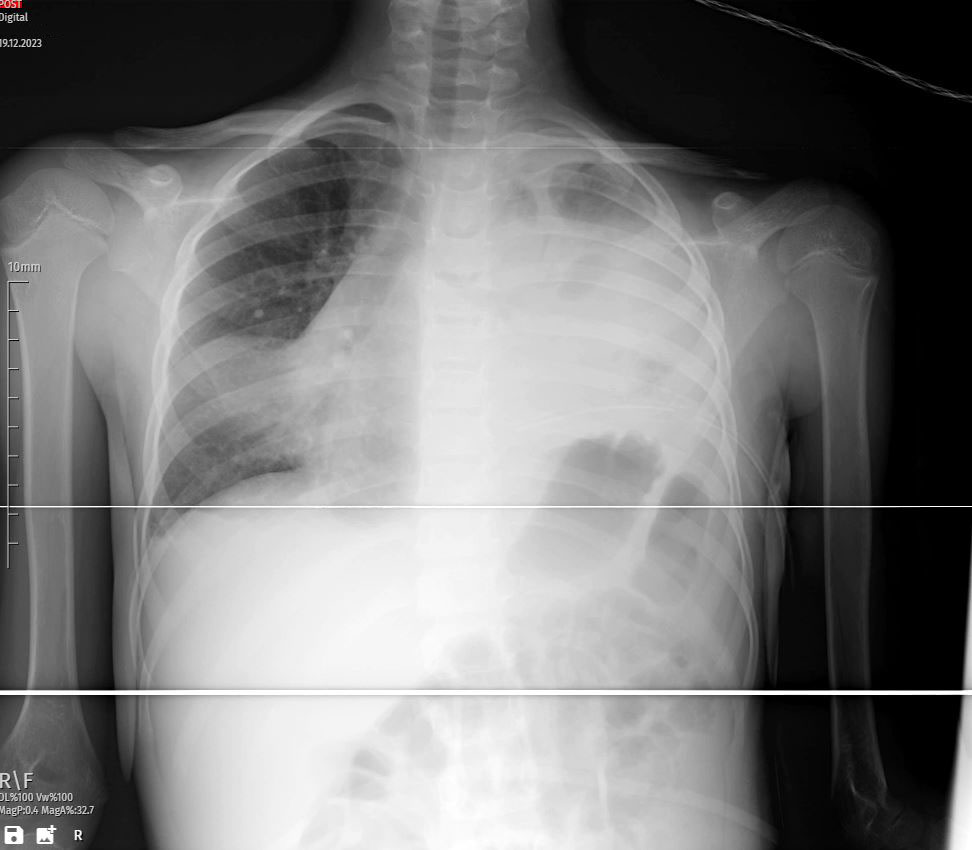
Follow-up X-rays on the second day illustrated a worsening condition, emphasizing the urgent need for intervention. Respiratory distress became more apparent, leading the medical team to initiate close monitoring and consider additional diagnostic measures to identify the underlying cause.
Day 6 – Thoracostomy and Antibiotic Treatment:
Given the escalating pleural effusion, a decision was made to perform a thoracostomy. This procedure involved the insertion of a tube into the left lung to drain the accumulating fluid. Simultaneously, a targeted course of antibiotics was initiated to address any infectious etiology contributing to the pleural effusion. The combination of drainage and antimicrobial therapy aimed to tackle both the symptoms and the root cause of the condition.
Day 9 – Improvement in Pleural Effusion:
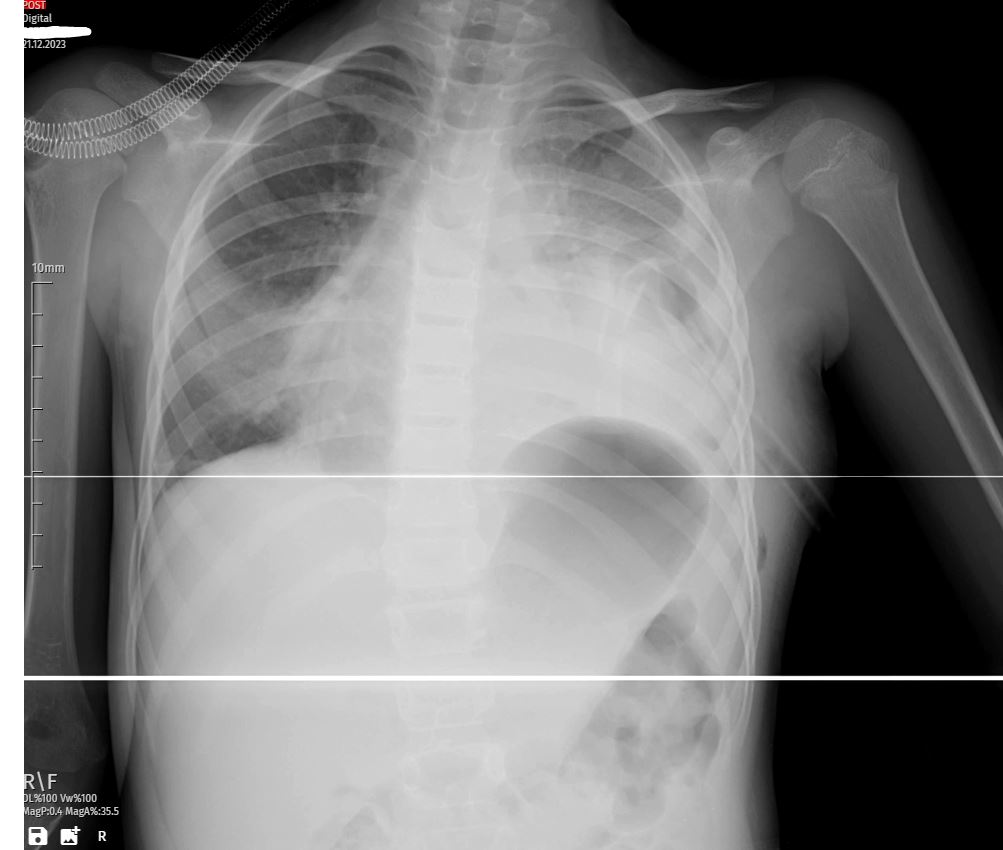
Follow-up X-rays on the fourth day revealed a positive response to the thoracostomy and antibiotic treatment. The white shadow on the left lung had visibly reduced, and the patient’s respiratory distress began to alleviate. The medical team continued close monitoring to ensure sustained improvement and adjust the treatment plan as needed.
Day 12 – Tube Removal:
With the patient showing significant improvement, the medical team decided to remove the thoracostomy tube. Subsequent X-rays confirmed a notable reduction in pleural effusion, supporting the decision to discontinue drainage. The transition from active intervention to a more conservative approach marked a critical phase in the patient’s recovery.
Day 15 – Discharge and Complete Recovery:
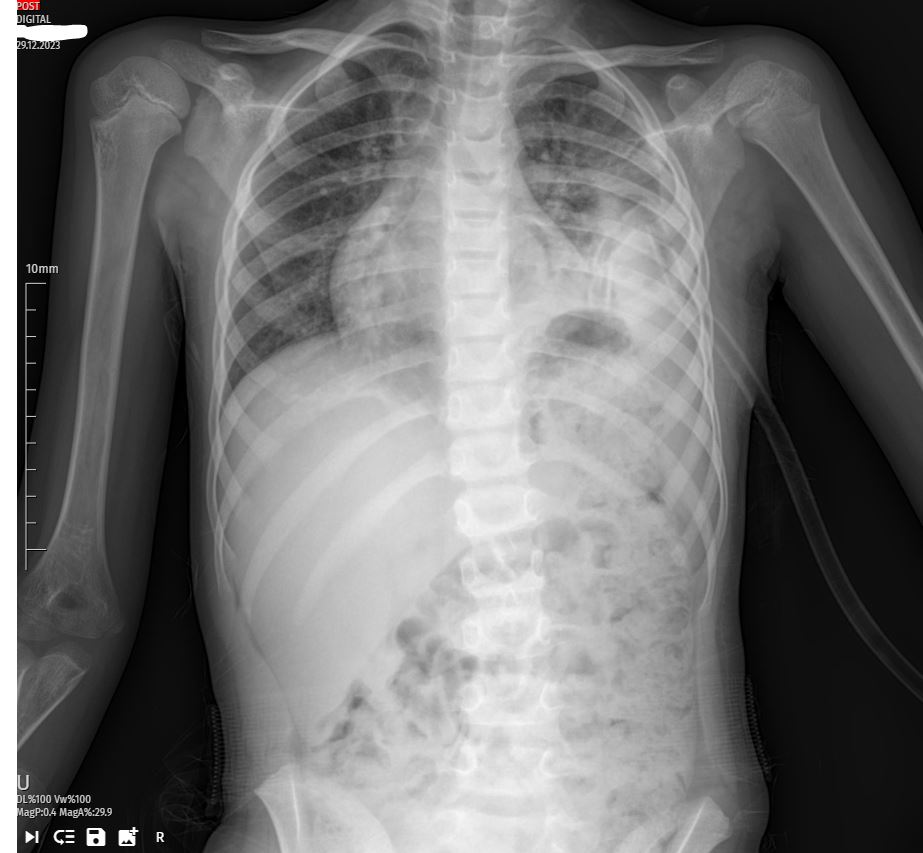
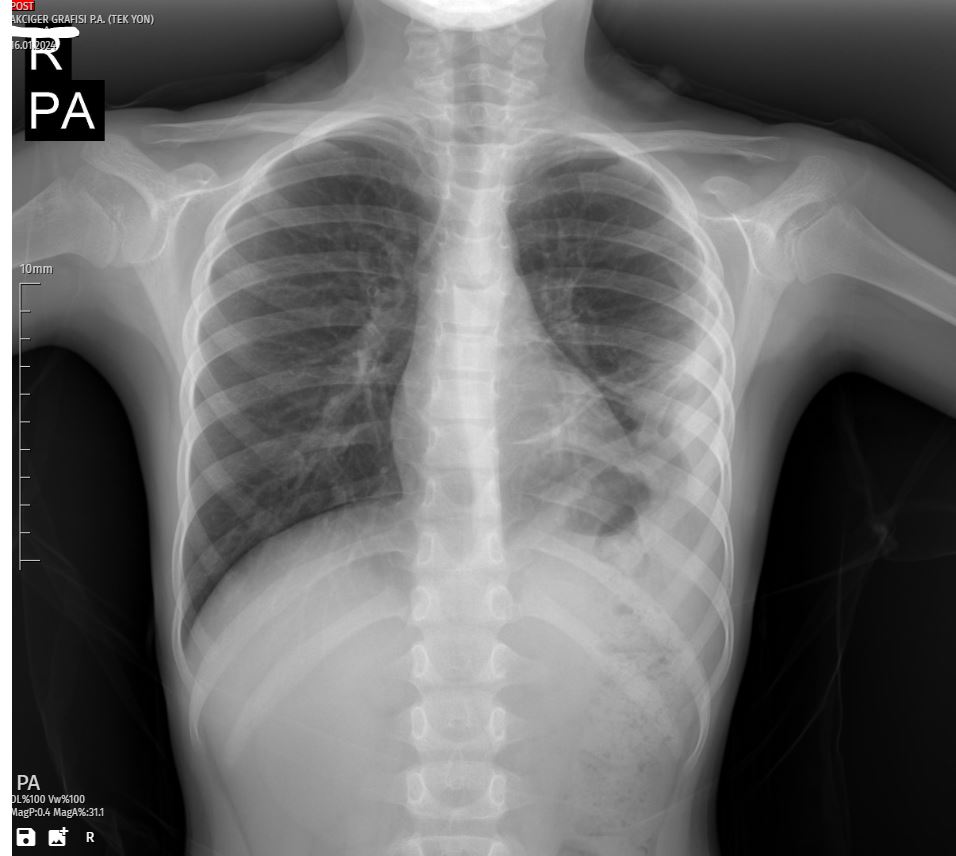
The final X-ray on the sixth day showcased a further improvement in lung condition, and the patient was deemed fit for discharge. The successful management of pleural effusion in this pediatric case underscored the importance of a multidisciplinary approach, including timely intervention, meticulous monitoring, and adaptive treatment strategies.
Understanding Pleural Effusion:
Pleural effusion arises from the accumulation of fluid in the pleural space, often triggered by underlying conditions such as infections, congestive heart failure, inflammatory disorders, or malignancies. Recognizing the common symptoms of pleural effusion, including cough, chest pain, and breathing difficulties, is crucial for early diagnosis.
Diagnostic tools such as X-rays and ultrasound aid in confirming the presence and severity of pleural effusion. Treatment strategies are tailored to address the underlying cause, and in severe cases, interventions like thoracostomy may be necessary to drain excess fluid. Antibiotics are prescribed when infection is suspected, highlighting the importance of a precise and comprehensive treatment plan.
Conclusion:
This detailed case study emphasizes the successful management of pleural effusion in a 6-year-old girl through a combination of thoracostomy and antibiotic therapy. The intricate journey from initial presentation to discharge underscores the critical role of timely and adaptable interventions, providing valuable insights into pediatric pleural effusion management. A comprehensive understanding of the causes, symptoms, and treatment options for pleural effusion is essential in delivering effective care, particularly in pediatric cases where prompt action significantly influences outcomes.