Clinical Summary:
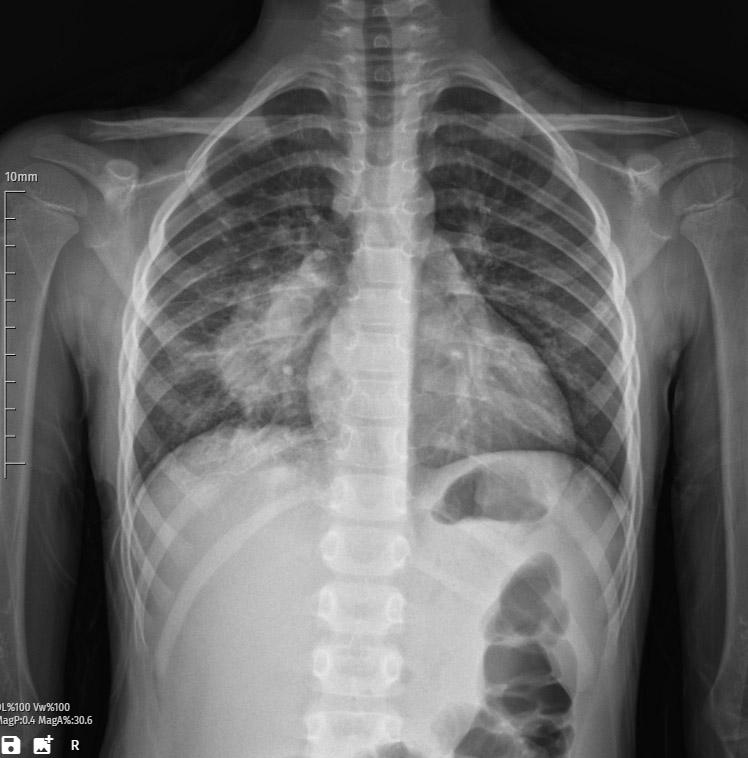
The patient’s chest X-ray reveals a consolidation image within the right lung, indicative of pneumonia. Consolidation refers to the solidification of lung tissue typically caused by infectious processes, and in this case, pneumonia is the underlying etiology.
Radiological Findings:
The X-ray displays opacification and increased density in the right lung, consistent with the presence of inflammatory infiltrates. The airspaces are filled with exudate, inflammatory cells, and debris, contributing to the observed consolidation pattern. This radiographic manifestation is characteristic of bacterial, viral, or other microbial-induced pneumonia.
Anatomical Localization:
The consolidation is confined to the right lung, signifying a unilateral pulmonary involvement. The affected area may exhibit loss of normal lung architecture, such as air bronchograms, due to the infiltration of pathological substances.
Pathological Changes in Lung Tissue:
Microscopically, pneumonia is associated with inflammatory changes in the alveoli and interstitium of the lung. There is an influx of neutrophils and macrophages into the alveolar spaces, leading to consolidation. The alveoli may be filled with proteinaceous fluid, pus, and cellular debris, impeding normal gas exchange.
Clinical Implications:
Pneumonia, as indicated by the consolidation on the right lung, suggests an acute inflammatory response within the pulmonary parenchyma. It is imperative to determine the specific microbial agent responsible for the infection through further clinical evaluation, such as microbiological cultures, to guide appropriate antimicrobial therapy.
Differential Diagnosis:
Differential considerations for consolidation on X-ray include bacterial pneumonia (commonly caused by Streptococcus pneumoniae, Haemophilus influenzae), viral pneumonia (such as influenza or respiratory syncytial virus), mycoplasmal pneumonia, and less commonly, fungal or parasitic infections. Non-infectious causes like pulmonary infarction or hemorrhage should also be considered.
Antibiotic Options for Treatment:
The choice of antibiotics should be guided by the suspected pathogen and local resistance patterns. Empirical treatment often involves broad-spectrum antibiotics such as ceftriaxone or cefotaxime combined with azithromycin or doxycycline to cover common bacterial pathogens. If the patient has risk factors for specific organisms (e.g., recent hospitalization), consideration of broader-spectrum agents like vancomycin or levofloxacin may be necessary.
Recommendations:
- Initiate Prompt Antibiotic Therapy: Begin empirical antibiotics promptly to cover likely pathogens. Adjust the regimen based on microbiological results.
- Monitor Respiratory Status: Assess oxygenation and consider supplemental oxygen to maintain adequate oxygen saturation.
- Diagnostic Investigations: Conduct further diagnostic tests, including blood cultures, sputum cultures, and molecular tests to identify the causative pathogen.
- Assess Overall Clinical Condition: Monitor for complications such as respiratory failure, sepsis, or pleural effusion, and adjust the treatment plan accordingly.
This radiographic presentation underscores the importance of a comprehensive clinical evaluation to tailor an effective management plan and optimize patient outcomes.